Is Percutaneous Discectomy Better Than Traditional Discectomy?
In this video/blog, we’ll be discussing percutaneous discectomy.
Procedure
In medicine, percutaneous refers to any procedure that’s performed by a needle through the skin. For a percutaneous discectomy, a thicker large diameter needle and small tools are used to remove the herniated disc. Most patients only have a small incision from the needle following the surgery.
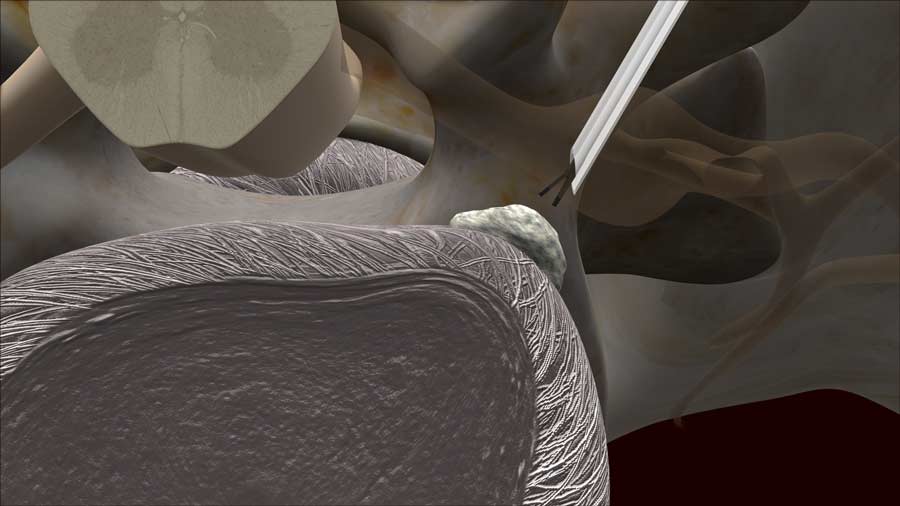
Usually, the patient is sedated, but not completely asleep. Using x-rays as a guide, the surgeon will pierce the skin with a skinny needle and carefully place it into the disc. Because the patient is awake, feedback will help prevent irritation of the nerve while placing the needle. In other words, pain will guide the surgeon away from the nerves. The skinny needle is used as a cannula to guide a thicker diameter needle into the disk. It is like a small straw being placed over the skinny needle. After the straw is confirmed to be in the disc, instruments then can be passed through to remove the disk material that is thought to be causing the pain. Nuanced differences in the techniques can utilize traditional graspers, suction devices, camera assisted visualization, lasers and other high tech or modern sounding instruments. In the end the result is the same: the removal of the herniated disc material.
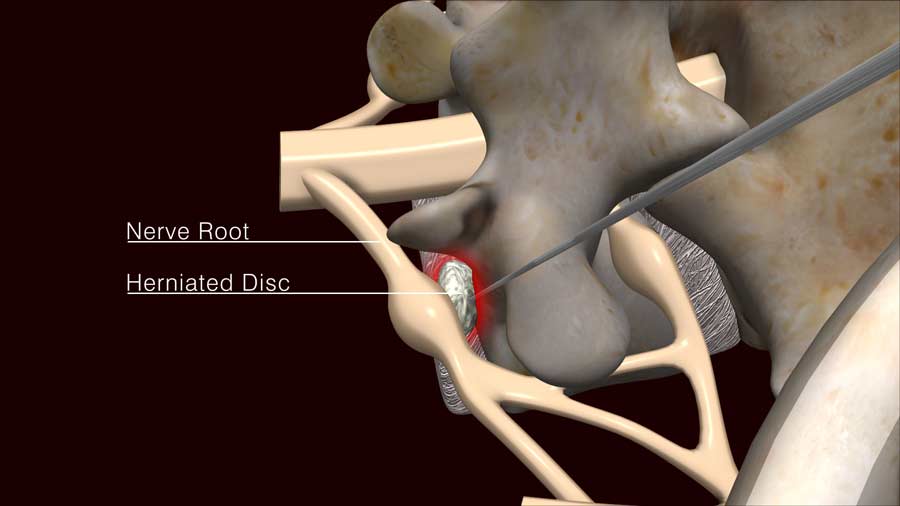
Unfortunately, it’s not as simple as it sounds. The outcome of percutaneous discectomy is not as predictable as most surgeons would like.The reasons are many. The percutaneous discectomy option is often considered because the disc herniation is not as large, and the physical examination findings are not as definitive. Percutaneous discectomy is thought to be the less invasive and therefore the less risky option. Because of that reason, many who would not normally choose open incision surgery will pursue this option. Surgeons know that people with a large disc herniation and the perfectly matching physical examination findings of corresponding numbness, reflex changes, and weakness will have the best predictable outcome. In this ideal scenario, formal open incision microdiscectomy is the operation of choice with the best results. Percutaneous discectomy is offered for the less predictable scenarios, thus with less predictable results. Then there is the issue of knowing whether the offending disc material has been adequately removed, as the visualization is not always optimal.
People forget that the perceived lower risk of the percutaneous option is not taking into account the risk of continued pain after surgery.
Review
A 2018 study examined patients who had a form of percutaneous discectomy. There were complications including incomplete removal of the herniated disc, nerve root injury, dural tear, and recurrence of the disc. These minimally invasive procedures are appealing to many patients because of their small incision and quick recovery. It does not mean there are no risks.
As in all surgery, proper patient selection and experienced surgical skills favor satisfactory outcomes. This is also reiterated in a recent 2020 study that states the steep learning curve for surgeons, and the lack of relevant experience contribute to the lack of predictability when it comes to percutaneous discectomies.
Conclusion
As with all surgical procedures, there are risks and potential complications. Please have your surgeon discuss the expected outcomes as well as further treatment options if the surgery does not result in improvement of your pain. And, most importantly, before you pursue any surgery, make sure you have exhausted all the non-surgical options. This part sounds scary, but it is a truth that few want to hear: There can never be a guarantee.
While Surgery can be a great option for those with well defined disc herniations, and matching physical examination findings, know that the goal should be to reduce your pain, and to return you back to normal activity, not specifically about the technique on how to achieve that goal. I know when the pain gets to be a frustration, the appeal of a surgical solution is great. But please remember there are risks, benefits and alternatives to all treatments. Make sure you understand them before signing up for any surgical option.
Until next time, this is Dr. John Shim.
Citations
- Pan M, Li Q, Li S, Mao H, Meng B, Zhou F, Yang H. Percutaneous Endoscopic Lumbar Discectomy: Indications and Complications. Pain Physician. 2020 Jan;23(1):49-56. PubMed PMID: 32013278
- Zhou C, Zhang G, Panchal RR, Ren X, Xiang H, Xuexiao M, Chen X, Tongtong G, Hong W, Dixson AD. Unique Complications of Percutaneous Endoscopic Lumbar Discectomy and Percutaneous Endoscopic Interlaminar Discectomy. Pain Physician. 2018 Mar;21(2):E105-E112. PubMed PMID: 29565953
Last modified: October 6, 2021









