20 years Cervical Spine
What happens to the disks in your neck over 20 years?
In 2018, Dr. Kenshi Daimon published a research paper addressing that question. I am going to summarize the findings.
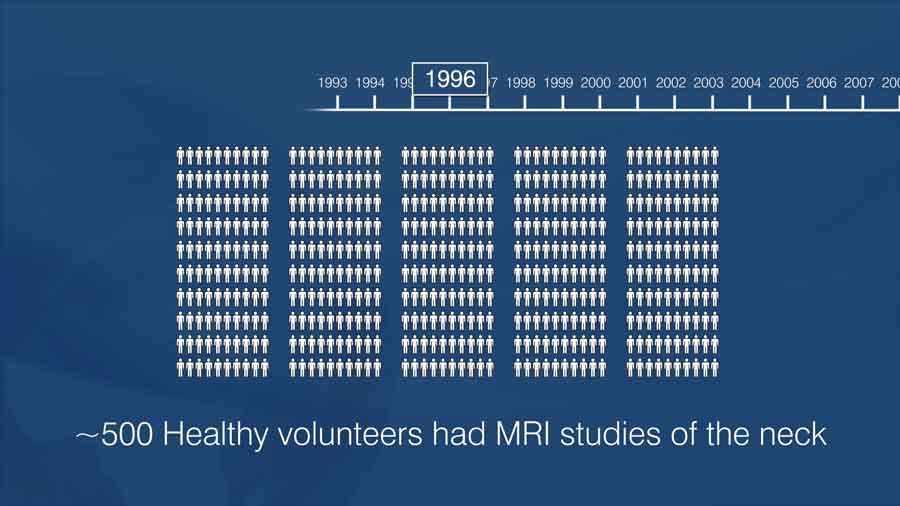
- From 1993-1996, about 500 neck pain free healthy volunteers had MRI studies of the neck.
- After 20 years, Each volunteer was then asked to obtain a repeat neck MRI, and answer a questionnaire about their current complaints. Anyone with a neck injury was excluded from this followup study.
- The original group of volunteers had age ranges from the teens to the early 70s. Of the original approximately 500 volunteers, 193 did consent to obtain both the MRI and answer the questionnaires. The research paper goes into details about the nature of this 193 subject group, and rationale for why this group was representative of the volunteer experience. The paper will be referenced below if anyone is curious.
- The information is consistent with what most practicing spinal specialist seen in their practices. Younger people had much less degeneration than older people.
- The C5-C6 level wears out first, with identified x-ray and MRI findings before the other levels.
- In 95% of the volunteers who completed the studies, there was wear and tear of at least one disc in the neck.
- In 60% of the volunteers, most of the disks to the neck also showed evidence of wear and tear over 20 years.
- For those over the age of 40, after 20 years, more than 80% had MRI findings of progression of spinal compression with disc protrusion.
- From the standpoint of the questionnaire, after 20 years, 45% had stiff shoulders, 18% had neck pain, 13% had headaches, 9% had numbness to the arms, 8% had ringing of the ears, and about 5% actually had arm pains.

So what this information mean?
The common sense part is that older people have more wear and tear. But, most important is that people without neck pain will wear out over time, and complaints such as stiffness of the shoulders, neck pain, headaches, and numbness happens with the aging process. Remember, this was in a group of subjects who did not have any known neck injuries.
Over 20 years, 95% will have increasing wear and tear of at least one disc level. This is the aging process.
From the standpoint of a surgeon, this paper confirms that many people will have evidence of spinal impingement and disc protrusions as the age. Very few will actually require surgical management. Very few are actually significantly symptomatic from these findings. The paper did suggest that development of foraminal spinal stenosis did have increased association with arm radiating pains. This paper then leads to more questions. Why does not wear and tear lead to more significant symptoms?
If discs naturally degenerate over time, does injuries change the nature of disc degeneration, or the development of complaints after disc degeneration?
Is this a Japanese genetic population experience or does this information also reflect conditions of other ethnic groups?

Aging is a gradual process. The body is able to accommodate the slow changes. Perhaps that is why we will have these findings as we age, but few of us will require aggressive treatments such as surgery.
At the same time, we do know there are things that will accelerate this degenerative process. Smoking, excessive weight, and poor diet can create a poor environment for our body cells, accelerating the aging process. We must do what we can. We do have some responsibility for our own aging process.
With each birthday, we get older, and wear out more. Accept it. Do what you can to slow down the aging process. Accommodate the changes and enjoy the cycle of life.
If you would like more information about spine topics, Please subscribe to Our newsletter or our YouTube channel.
Last modified: May 5, 2020









