Cervical Selective Nerve Block
What is a Cervical Selective Nerve Block?
For people with arm pain and tingling secondary to a pinched nerve in the neck, most of the time, the pain does get better. But for a small minority, the pain remains constant despite all conservative treatments.
For those people, your physician may offer injections of cortisone to the neck. The rationale being, the cortisone will help decrease the inflammation on the nerves. With reduction of inflammation, the pain, tingling and numbness may improve.
These injections have many names, and many forms. Cervical epidural steroid injections. Cervical Nerve Block. Cervical Facet Injections.
The effects of the cortisone is secondary to its very potent anti-inflammation effect on tissues. Any nerves or tissues that are swollen can potentially decrease in size with the cortisone effect. Remember that cortisone is a steroid, and some forms naturally occur in the body. But, with concentration of the steroid (cortisone), most tissues will decrease its inflammation.
In addition, by delivering a solution near the area of inflammation or injury, the fluid can help dilute the various concentrated enzymes, and painful substances, that are causing the irritation in the limited spaces of the spine.
Cervical Selective Nerve Block have one more function. In certain situations, there may be confusion as the cause, or location of the nerve compression or “pinched nerve”. In the more typical situation, a person has physical findings and MRI evidence of multiple pinched nerves. As we try to isolate which of these nerves are causing the pinch, we can use Cervical Selective Nerve Block to differentiate the pinched nerves identified on the MRI versus the pinched nerves that are actually causing the pain. As some of you may know, many times, nerves can be pinched, but not have any associated pain, numbness or tingling.
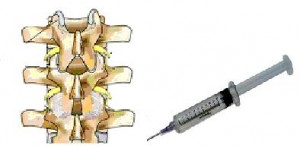
In the process of Cervical Selective Nerve Block, the physician will direct a small needle next to the nerves of interest. Then, usually one at a time, as close as possible to an individual nerve, a small amount of a fluid similar to novacaine, along with a small dose of cortisone is delivered onto the nerve. Then a certain amount of time passes to see if the Cervical Selective Nerve Block causes improvement of the pain and discomfort associated with that particular nerve. Then, a second, and possibly a third nerve is injectioned to see if the nerve has improvement with the Cervical Selective Nerve Block. The key is to deliver a very small amount of the novacaine/cortisone fluid to each nerve so that it will only effect that nerve.
With the results of Cervical Selective Nerve Block, the cause of the pain can be isolated to the truly affected nerve. This sometimes makes a significant difference in determining the type of surgical procedure necessary to correct a chronic and severe pinched nerve in the neck. This technique can also be utilized in the lower back as well, with associated sciatica.
Though the process sounds a bit intimidating, Cervical Selective Nerve Block can help isolate your problem, and improve your surgical outcome.
Citations
- Jonayed SA, Kamruzzaman M, Saha MK, Alam S, Akter S. The Role of Selective Nerve Root Block in the Treatment of Lumbar Radicular Leg Pain. Mymensingh Med J. 2016 Jan;25(1):141-7. PubMed PMID: 26931264
- Eastley NC, Spiteri V, Newey ML. Variations in selective nerve root block technique. Ann R Coll Surg Engl. 2013 Oct;95(7):515-8. PubMed PMID: 24112500
Last modified: January 5, 2018










At our London Clinic we regularly treat post-surgical back pain. As a conservative based clinic we welcome diagnostic nerve blocks as a method of identifying the active disc prior to surgery. Far to often it is difficult to isolate the active disc leading to poor surgical success and poor patient satisfaction.
I agree with your general sentiment. As you know, outcomes for lumbar or lower back procedures are not as good as cervical or neck procedures. In our experience, we also see similar effects regarding diagnostic nerve blocks. In the neck, there is a greater chance that we will identify the potential cause of the problem, and can offer a surgical option with greater chance of success. In the lower back, not so much. While many of my younger, or more aggressive colleagues will still try to surgically manage many of the patients that do not respond to these injections, I find that the more experience I gain, the less likely I will offer a lumbar surgery, especially a lumbar fusion.
I also tend to steer away from spinal fusion unless there is instability. We are working more frequently with upright MRI scanning machines which take into account posture, weight and movement. The results are quite outstanding! Being a chiropractor who has had a lumbar microdiscectomy I offer a unique understanding.
London Chiropractor,
Thanks for commenting on my post. I am intrigued by your perspectives and hope you continue dialogue. If you are on Google +, I invite you to join my Google + Spine Surgery community.