COVID-19 and Bone Fractures
What are the risks of having both the COVID-19 infection and having a broken bone?
As of today, April 15, 2020 the United States remains in a state of social distancing and businesses are shut down except for essential services.
Even elective surgery is not permitted in the State of Florida in order to save ventilators, medical equipment and medical beds for potential COVID-19 infection patients. Only emergency surgeries for certain broken bones, nerve compressions and infections are being performed. The effects of surgery on COVID-19 patients on an emergent basis is a significant concern.
So far, much of that experience on treating broken bones on patients with the COVID-19 Pneumonia infection has been in China, as the Pandemic experience is several months ahead of the USA.
Orthopaedic Surgeons in Hubei Province China have recently shared their results in caring for 10 COVID-19 patients with broken bones in the JBJS express publication. The lead Author is Dr. Bobin. Of these 10 patients, 7 had broken hips. 2 broke their spine. One broke the wrist.

Before I review the Hubei experience, the viewers should know that large bone fractures such as broken hips, and broken spines are associated with breathing problems. There are three main reasons:
- These breaks are very painful, and limits the ability to situp or mobilize, thus reducing breathing capacity.
- Older patients typically have broken hips. The cause being osteoporosis, and generalize physical decline.
- Breaks of large bones can release fat droplets in the blood, which can block the lung micropores, and reduce the inflow of oxygen.
Even without the COVID-19 infection, these folks are already at high risk of complications, poor outcomes and death. Yearly mortality rates for broken hips in the geriatric population is up to 35% in the first year.
Unfortunately, the outcomes are even worse if you have the COVID-19 Pneumonia.
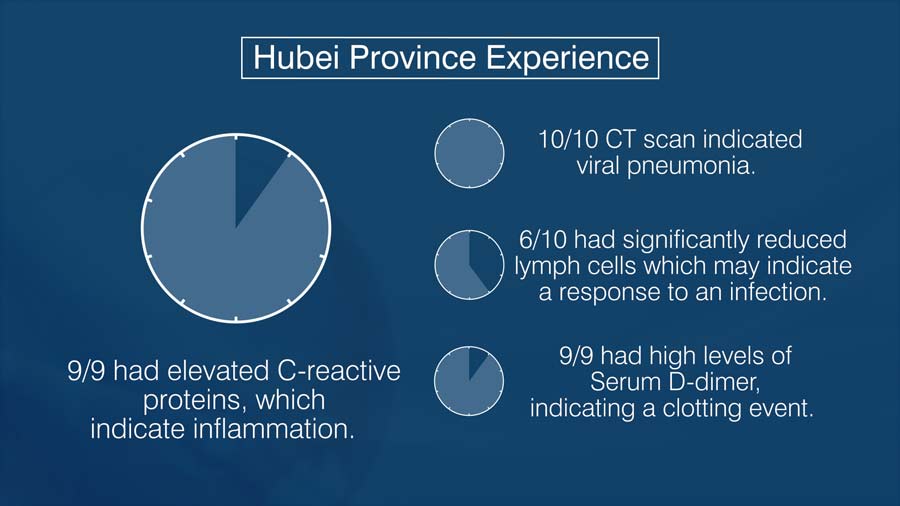
In the Hubei province experience, all 10 patients had CT scan evidence of the viral pneumonia.
6/10 had significantly reduced lymph cells which may indicate a response to an infection. 9/9 had high levels of serum d-dimer, indicating a clotting event. 9/9 had elevated C-reactive proteins, which indicate inflammation.
Of these 10 fracture patients, 3 had surgery. 7 were too sick to have an operation, or the doctors decided that non surgical treatment was the less risky approach.
4 patients died within 2 weeks of admission. All of these patients were older than 75 years of age.
The remaining 6 patients longer term outcomes are yet to be determined. Most of the surviving patients were younger than 55 years old. At the time of presentation of this information for publication, these patients were listed as remaining in the hospital.
All patients received anti biotics and anti viral medications.
In this small sample size of patients, those over the age of 75 had a 66% mortality rate 2 weeks after admission to the hospital.
Of the three patients who had surgery (all for broken hips), one died.
The authors of the paper did provide some standard suggestions about infection protocols, caution on offering surgery, and the recommendation for use of a negative pressure operating room.
From my review of the limited data, the high mortality rates are associated with advanced age, concurrent medical issues such as respiratory disease, cirrhosis and brain injury.
Broken bones in those who have advanced age and in combination of medical conditions is already a very high risk situation.
With a COVID-19 pneumonia, the risks get compounded, and the mortality rates are worse compared to the mortality rates without the Virus infection.
I know the sample size is very small,
The Hubei Experience is very sobering. I share concerns for all patients who have COVID-19 infections, and urge all to follow the health department recommendations of your local governments.
I do not want to alarm you all. I just wanted to share the upcoming Publication in the JBJS about the COVID-19 virus and Fractures.
Last modified: April 22, 2020









